
06 Apr William’s Birth Story | Brisbane Birth Photographer
I saw a quote the other day that really summed it up for me – “Your first breath took ours away.” Almost six months later, I can still distinctly remember the moment Karen’s doctor said “Bring your hands to me – one more push and I’ll hand you your baby.”
Nothing that quite compares to being there for the arrival of a brand new, tiny human.Being part of William’s birth was so special, and Karen has very generously allowed me to publish William’s birth story along with the images from her labour.
In her own words, this is not a “nice” story – but it is beautiful, emotional and very honest.
So grab a couple of tissues, and let Karen introduce you to her son.
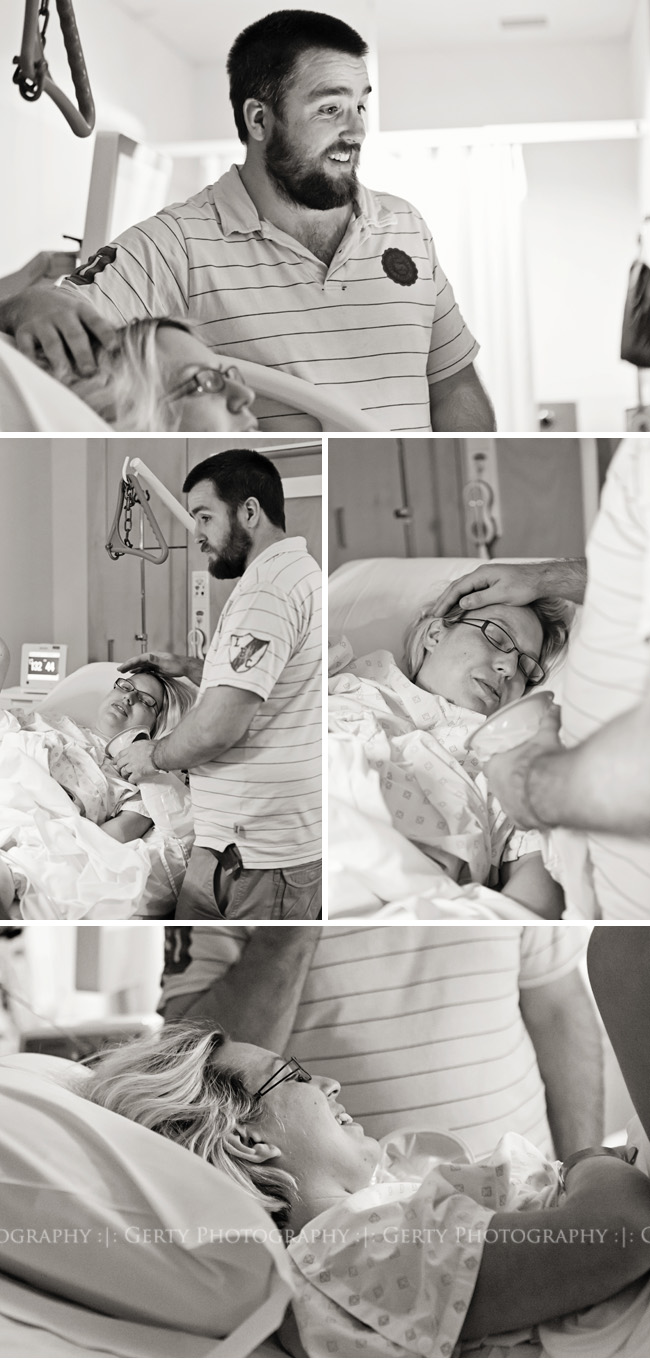
William’s birth story – written at 3 weeks post birth:
I woke around 3am on Saturday, 20 October, desperately needing to go to the toilet for a number 2. I woke again not long after with the same feeling. And again and again. Soon my bowels were empty but the pressure was so intense I realised that this was it: labour had begun. And my first thought was “If this is the start, I’m going to need an epidural before the end!”
I had read the Hypnobirthing book and really wanted to have a drug and intervention free labour. I believed the stuff in the book about how a calm birth is beneficial for a baby and how a traumatic birth more likely leads to complications. I’d seen the US ‘One Born Every Minute’ and DH (Dear Husband) well knew what I thought about women who lie on their back with their legs up in stirrups when trying to deliver.
The morning went well, contractions were getting stronger and more regular but I was breathing through them. I spent a few hours playing the piano and singing – I love my music and it is a great distraction. The fit ball was great too. By late morning the contractions were more regular and DH started to get a bit nervous so we headed into hospital.
I was only 3 cm dilated and 2/3 effaced but the Mater Mothers Private Hospital in Brisbane has a ward where you can wait for active labour to begin if you don’t want to go home. We thought we’d stay as we were a bit nervous about knowing when to come back. We had a private room with a shower and everything so we were very comfortable. I stayed in the shower for hours, again, singing to myself and my baby. It helped with the back pain so much! I didn’t have any other pain, just this intense pressure on my bowels.
Evening came round and I was still only 3cm. I was beginning to struggle though – the back pain was becoming unbearable and the shower no longer helped. Baby was posterior – the thing I had spent so many hours at the pool trying to fix! I knelt on the bed with DH trying to remind me to breathe and just yelling at him “fuck that hypnobirthing shit!” I really, truly thought my bowels were going to explode out of my body and I would be permanently damaged.
By 7pm I was starting to lose it but the midwives still didn’t think I was in active labour. They suggested pethedine to give me some rest (read: it’s going to take a lot longer yet!) – my birth plan said “NO PETHEDINE!!”. That was the first thing to go: I needed rest. I took it, I got some, but I also spent an hour feeling very woozy and in pain. I lost track of the time by then, but around midnight I lost it and begged for the epidural and they took me down to the birthing suite.
I dropped my bundle: I completely lost it! I still feel a bit traumatised about all the people around me, DH shoving the gas in my mouth trying to calm me down, and the anesthetist trying to get the epidural in. I was in so much pain and I no longer cared about my ‘calm birth’.
Things went fairly quickly from there – I had dilated 4 cm in the time it took to get to the birth suite. They broke my waters and I was fully dilated in no time. They put my legs up in stirrups as I lay on my back and they told me to push. Nothing was happening the way I wanted it too but it was out of my hands now. That was the price I paid for the relief of the epidural, and I suppose it was worth it. I couldn’t feel anything to push though, and I really wanted to ‘breathe’ the baby out. They wouldn’t let me, but I couldn’t feel to push! The baby’s heart rate was rising and falling and I knew I didn’t have very long before they’d want to intervene again and I really didn’t want to have a c-section. I suppose it was with a degree of relief that the intervention that came was only the vacuum suction. I breathed him out then, and in two breaths he fully emerged – the most incredible thing I’ve ever seen! Little William, named after his great grandfather, and born on his great grandfather’s birthday!
While they stitched me up (2nd degree tear plus an episiotomy), I gave William his first feed – the boy knew what he was after! By 6:30 am we were settled in our room, the three of us exhausted but very happy.
Sunday and Monday were beautiful days with our little boy. DH was about to head home on Monday night, I was about to go to sleep and the midwife was just checking in on us when William coughed up some blood. I thought that’s probably normal but the midwife called the paediatrician anyway. He brought up a little more…I wasn’t too concerned…and then he did an almighty vomit and brought up a bright red pool of blood. I immediately burst into tears, the midwife rushed him to the RESUS room and all the nurses converged. They rushed him down to NICU and told us to wait in our room while they got the drip into him. We waited, the two of us crying uncontrollably.
The doctors didn’t know what was wrong but started him on a few different medications and ran a number of tests. His poor little body was beginning to shut down so they really struggled to get an IV in. By the time we went down to NICU later that night he was covered in bruises from them trying to get a line into any vein they could.
By morning they were even more concerned because he had passed so much blood through his bowels overnight. They were going to do an endoscopy later that day to try and work out what the problem was. I went into shock and shut down – I don’t really know what happened that day. DH spent the day in NICU introducing William to family members who hadn’t seen him yet, I went back to my room and screamed and moaned and cried and cried and cried. I kept expressing although it was so hard – William would need the milk soon. Surely. DH wanted to know all the possibilities and processes of elimination. All I knew was that my baby wasn’t with me – and that hurt so much more than labour!
By the afternoon the hospital had arranged for all the potentially relevant specialists to be in theatre. They asked us to sign an open consent, allowing them to do pretty much whatever they deemed necessary. The look on William’s face as he looked up at me out of his humidicrib just broke my heart. There was nothing I could do for him and I felt so helpless. I can’t describe the horror I felt as they took my precious boy away to theatre, not knowing what was going to happen.
While we waited my milk came in but I had nowhere to express. I missed my pain medication too so my stitches began to hurt. But before too long the paediatrician came bouncing into the waiting room – it was stomach ulcers! Extraordinarily rare in a new born, but easily treated! In fact, the medicine they had started him on the night before was already working.
None of the midwives had ever seen something like this and even the gastrologist, who spends his whole life looking into babies’ bellies – and sees all the special cases from SE Qld – said he would see this about once every 4 years!
William had lost a lot of blood and was literally as white as his sheets. They were monitoring him closely to decide whether or not he needed a blood transfusion. No one knew what would have caused it but I did hear a couple of references to ‘stress ulcers’ and the ‘stress of childbirth’.
Oh God, this was my fault! The Hypnobirth book was right – if you fail to give your baby a trauma-free birth bad things will happen! I should have paid the $300 to do the class and learn how to give birth properly; I should have had more faith in myself that I could do it; I should have exercised more during pregnancy so he wasn’t posterior. I couldn’t stop blaming myself.
One of the midwives really took me under her wing – she genuinely cared about me. She helped me see that ulcers don’t form that quickly. She said she looked at the notes from my labour, thinking it must have been really horrible, but she said my labour was really quite standard. And if the stress of labour causes ulcers, we would see it in every second newborn. She got me to see the psychologist and really prompted me to be proactive about my mental health. She was saying seeing my baby throw up so much blood and the whole experience was likely to give me post traumatic stress which could easily become post natal depression.
William is fine now. He’s on medication and iron supplements for the next few months. The paediatrician explained that a blood transfusion was an absolute last resort because giving blood to a new born interferes with their ability to produce their own blood. It was touch and go for a while but he avoided the blood transfusion. We owe so much to all the midwives and doctors at the Mater: they took such good care of us, not just physically but emotionally too. I’m feeling strong and supported by DH, but we’re going to get a referral for the government’s PND ATAPS program anyway. Just in case.
We love William so very, very much.












No Comments